Imprisonment of TB Patients Declared Unconstitutional in Kenya
By Allan Maleche & Timothy Wafula
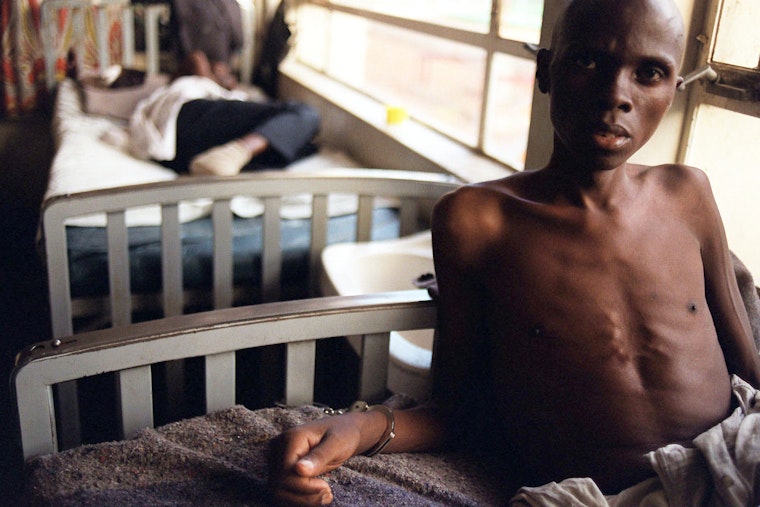
On August 12, 2010, Daniel, Henry, and Patrick, residents of Kenya’s Nandi County, were arrested for default—not on a debt, but on a disease. They were charged with failing to maintain their prescribed medical treatment for tuberculosis (TB). Daniel and Patrick were brought before the principal magistrate at Kapsabet Court. Henry, in poorer health, was admitted as a patient at Kapsabet District Hospital.
Daniel and Patrick were convicted and sentenced to eight months in prison. Behind bars, they slept on the floor without bedding for over a week, shared crowded cells with other inmates, and were denied the balanced diet required by TB patients on medication. They served 46 days of their prison terms before civil society organizations secured their early release.
As outrageous as these cases seem, they are far from isolated. There have been many others, both reported and unreported, in which Kenya’s Public Health Act was invoked to incarcerate TB patients who defaulted on their medications. Such arrests are in clear violation of the World Health Organization’s guidelines, which state that when involuntary isolation or detention of a patient is absolutely essential, it must never be implemented as a form of punishment.
KELIN, an organization established to protect and promote health-related human rights for all, noted these guidelines in its petition [PDF] on behalf of Daniel and Patrick, filed in the High Court of Kenya. In the petition, KELIN does not argue against the isolation of persons suffering from infectious diseases, but rather against their isolation in prisons.
Congested prison facilities subject sick people to poor nutrition and hygiene, putting them at risk of additional infections. They’re also blatantly punitive, and violate the constitutional threshold of reasonableness.
Housing people with infectious diseases in prisons is also dangerous for the community at large. No precautions were taken to prevent the spread of TB within the prison. And the complexity of TB treatment—four or more medicines administered over six to eight months—makes it vulnerable to improper administration, which can lead patients to develop a drug-resistant version of the disease.
“Not only is such action not sanctioned by the Public Health Act,” noted Justice Mumbi Ngugi in her ruling, referring to the incarceration of TB patients, “it is also patently counterproductive.”
On March 24, 2016—World TB Day—the High Court declared that the practice of incarcerating TB patients to be illegal and unconstitutional, and directed the government to develop a policy that incorporates international principles on handling the disease. In order to ensure these orders are implemented, the court took the unusual step of directing the government to file an affidavit within 90 days detailing the policy measures it had put in place.
This judgment is a game changer for Kenya. It will finally put a stop to the arrest and imprisonment of tuberculosis patients. It ensures that future isolations will be handled in a patient-centered manner that respects human rights. And it opens a channel for dialogue on how to achieve a rights-based approach to TB prevention, treatment, and management. Implemented successfully, Kenya’s new policy could act as a model for the region and beyond.
KELIN is a grantee of the Open Society Foundations.
Allan Maleche is a human rights lawyer and executive director of KELIN.
Timothy Wafula is a human rights lawyer working with KELIN on the rights of TB patients.


