The Overwhelming Evidence in Favor of Harm Reduction
By Katie Stone

Recently, in Bucharest, I visited one of Romania’s few programs left for providing methadone, an essential medicine for treating opioid dependence. The people I met explained the significant challenges of providing this service. Police harassment is common and resource shortages mean people are often forced to wait months to commence methadone. For those with a history of drug use, an HIV-positive test means prolonged suffering because of the government’s indifference to treating them.
Despite this program’s resilience in the face of hostility, the services were being pushed out of the building within weeks and staff were racing to find another site and continue medical care for clients. Unfortunately, this experience is not unique—stigma, political reticence and a lack of funding for harm reduction mean this plays out all over the world.
Of the more than 15 million people worldwide who inject drugs, over half live with hepatitis C, and nearly one in five live with HIV. These diseases are entirely preventable with harm reduction programs like needle and syringe programs and opioid substitution therapy. Yet the latest research from the organization where I work, Harm Reduction International, reveals that less than half of the 179 countries where injecting drug use is reported implement these health services. In the two years since we last reported, progress has stagnated.
Harm reduction is not just about responses to HIV and hepatitis C. It covers a range of public health and social interventions that aim to improve quality of life, and to uphold human rights and dignity. The use of amphetamine-type stimulants is reportedly rising worldwide, particularly in Asia, and countries are not adapting to this trend. The availability of information on safer use and safer smoking kits, for example, is scarce.
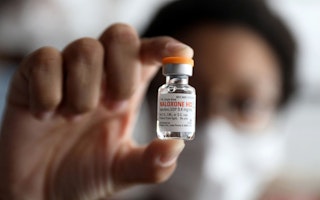
We also can’t talk about harm reduction without addressing the spike in opioid- and drug-related deaths across several regions—notably Canada, the United States, and the United Kingdom, which all saw record fatalities last year. Naloxone, a powerful medicine that reverses opioid overdose, is becoming more widely available. But pricing and prescribing barriers, along with burdensome regulations on who can carry naloxone mean that in many areas, the people who need it most can’t get it. Only 12 countries around the world allow peer-distribution programs.
Underpinning the gaps in harm reduction is a lack of political or financial will prevalent in most countries. At one end of the spectrum, societal and legal hostility toward drug use can create an environment where people with problematic drug use are unwilling to access services because of the stigma attached. At the other, it manifests in brutal crackdowns like in the Philippines, where at least 20,000 people have been executed in the country’s war on drugs since 2016.
Amidst this gloom, our report does pick out bright spots, breakthrough reforms, and the perseverance of activists, service providers and some policymakers. The number of countries implementing harm reduction in sub-Saharan Africa is creeping up, for example, and a leap in the availability of drug checking services in Latin America supports people to make safer choices. Canada is taking action to address its overdose crisis through the rapid opening of supervised injection facilities and pop-up overdose prevention sites to help keep people alive. At a local level, there are inspiring examples of holistic and gender-sensitive harm reduction programs for women who use drugs in Myanmar, Spain, and Mexico.
So what next? A good place to start, is for countries to redirect money from ineffective drug law enforcement to harm reduction. At least $100 billion is spent annually on drug control around the world (incidentally, in their 2018 report [PDF], the UN Office on Drugs and Crime noted that the drug trade continues to boom). Shifting just 10 percent of these funds into harm reduction could end AIDS among people who inject drugs, cover hepatitis C prevention for this population twice over, and fund enough naloxone to save thousands of lives.
The evidence for harm reduction services is overwhelming. They keep people alive, are cost-effective, and foster healthier, safer communities. It is shameful that these facts are ignored by many. Until prejudice and fear stop ruling when it comes to drug policy, our health will continue to be undermined.
Harm Reduction International is a grantee of the Open Society Foundations.
Katie Stone is a social science researcher who leads the Public Health & Social Policy team at Harm Reduction International.