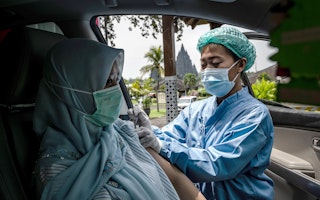
Q&A: Africa’s Fight for Vaccine Equity

Throughout the COVID-19 pandemic, vaccine nationalism and manufacturers prioritizing high-income countries severely limited the number of vaccines available to the majority of the world’s population, resulting in millions going to waste. While almost two out of three people globally have received at least one dose, only about 20 percent of Africans have—in part because of late and unpredictable access. Tian Johnson, founder of the African Alliance, a global nonprofit based in South Africa working on health rights issues, shared reflections on how to make progress in the push for vaccine equity as the world enters the third year of the pandemic—and what African civil society organizations are asking for now.
Deep inequalities persist in global access to vaccines, treatments, and diagnostics. What impact has this had on the ground?
If you are a teacher in Zimbabwe—or a number of other African countries—a COVID test will cost nearly half of your monthly salary. Six out of seven cases go undiagnosed on the continent, which not only results in the continued spread of the virus but will prevent individuals from being promptly treated once therapeutics become available. The lion’s share of treatments expected to become available this year has already been purchased by wealthy countries, even though it is low- and middle-income countries that need them most.
African countries’ inability to access the tools necessary to contain national epidemics and produce their own supplies has also increased national debt. Countries—many of which were already highly indebted—were forced to borrow more from international lenders to purchase vaccines. This has forced African nations to spend to save lives now at the expense of investing in developing essential services, including health care, education, and social safety nets that protect lives and livelihoods in the future.
As countries and the World Health Organization begin to invest in African vaccine manufacturing, what steps are needed to ensure that the continent builds pandemic preparedness and self-reliance for the future?
Interventions during the past two years to increase timely and equitable access to medicines for Africa have not addressed the root causes of inequality. For instance, donor funding for initiatives and voluntary licensing remains largely at the Global North’s discretion and ultimately curtails the agency of African countries and their pandemic preparedness. These measures fall dismally short of ensuring that African nations assert their sovereignty.
That’s why funding for local production in Africa must be free of strings and intellectual property provisions that will continue to benefit the pharmaceutical industry. This year, civil society groups in South Africa wrote to Moderna, calling the company out for continuing to keep the vaccine recipe—funded by public money, not pharma “goodwill”—a secret and making aggressive moves in Africa to keep that recipe out of the hands of manufacturers. This is why we must continue to center the discourse on the decolonization of global health and challenge the pharma greed that has resulted in us now facing another year of preventable COVID deaths.
The Africa Centres for Disease Control and Prevention has now become a catalyst for advancing discussions around local production that had, up until now, largely stalled at the African Union. As African leaders develop local manufacturing, governments must retain sufficient ownership of these new facilities to ensure their strategic direction and output serves the public interest first.
You’ve called on civil society to be relentless in seeking accountability around clinical trials to develop new medicines and vaccines to treat COVID-19, and clinical research in general. Why is this such an important issue?
Life-saving scientific discoveries that don’t prioritize and center access for all are unjust and must continue to be called out. The need to develop COVID tools quickly is now being used as an additional excuse for researchers to avoid funding and executing community engagement meaningfully.
In some cases, engagement has been limited to Zoom briefings and trial launch and closeout events. Moreover, it is common for communities to be engaged through an advisory board comprised of local representatives such as faith leaders, activists, and community health groups. That’s not enough. Instead, for the sake of accountability and transparency, local consultations should include a broader range of input from individuals who have no official affiliation with the trial.
All clinical trials should be implemented with well-resourced community engagement plans that span all phases of research, from protocol development to dissemination and access. To ensure that medical products will be effective and safe for equity-seeking groups, clinical trial participants must include women, including transgender women, and others who are traditionally underrepresented in medical research, such as people living with HIV.
Many researchers leading trials who partner with pharmaceutical companies are content to do so with few conditions to ensure that the community benefits from pharma involvement other than the promise of drug donations. But researchers need to go further and be clear that they will not support any research that does not come with clearly defined conditions for how the most vulnerable will access the results of that research.
From the onset of the pandemic, you and other African civil society leaders have called for a global cooperation model based on justice, not charity. What does this mean in practice?
The pandemic has shed light on the longstanding and violent inequalities between the wealthy and the poor, the have and have-nots—inequalities that COVID has exacerbated. G7 and EU leaders must include conditions on future research and development funding for medicines in response to pandemics to ensure that public financing achieves a public good, instead of enriching powerful pharmaceutical companies and adding to the rapidly growing pool of pandemic billionaires.
The African Union, G7, and other leaders must urgently agree to a fully funded roadmap to reach the World Health Organization’s goal of vaccinating 70 percent of the population in every country in the world against COVID-19 by mid-2022. COVID is not over until we have equitable access to vaccines, tests, treatment, and linkage to care.
A pandemic treaty—like the one currently being developed by the World Health Assembly—must ensure that any response to the current pandemic or future pandemics is grounded in the principles of community, equity, transparency, and accountability. That means, for example, including strong language barring the imposition of travel bans in line with the International Health Regulations. To prepare for the next pandemic, world leaders must also explore new research funding and development methods that de-link R&D costs and pricing to increase equitable access. We need a justice-driven pandemic preparedness strategy.
The COVID-19 pandemic has left an indelible mark upon the world. We will undoubtedly find ourselves pausing to mourn the millions of lives lost to this disease in the years and decades to come. Only then will we be ready to finally ask ourselves how many died needlessly due to the hoarding and profiteering that gave rise to one of the most preventable travesties in human history.
African Alliance is a grantee of the Open Society Foundations.