Training Drug Users and Bystanders to Treat Overdose Saves Lives
By Roxanne Saucier
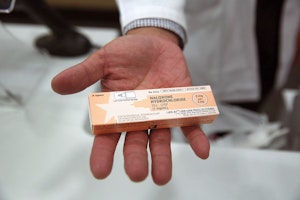
Drug overdose is a growing public health crisis that now kills more adults per year in the United States than motor vehicle accidents. In cars, seatbelts and airbags save lives. When it comes to opioid overdose a safe and non-abusable medicine called naloxone can restore breathing and avert death. Pragmatic doctors and health officials want anyone who uses opioids like heroin—and anyone likely to be around during an overdose—to have access to this life-saving drug, and know how to use it.
In Massachusetts, researchers led by Dr. Alexander Walley at the Boston University Medical Center set out to discover the results of a state-supported overdose education and naloxone distribution program on deaths from overdose. We sat down with Dr. Walley to discuss the findings.
What did your research find?
This study demonstrates that overdose education and naloxone distribution is an effective public health intervention to address the growing overdose epidemic. We found that communities that received overdose education and naloxone reported significantly fewer deaths than communities that received no training. We also observed that the higher the cumulative rate of program implementation, the greater the reduction in death rates. In other words, the more people at risk or in contact with people at risk for overdose who were given naloxone, and trained to prevent, recognize and respond to an overdose, the lower the overdose death rates.
Why are overdose education and naloxone delivery programs like these so important?
Since the beginning of the Massachusetts overdose education and naloxone delivery programs, there have been more than 1,700 overdose rescues using naloxone. While we do not know how many of these people may have died if they had not received naloxone, it is likely that many of them would have. These rescues have inspired many us to maintain hope that all overdose deaths can be prevented.
People who have recently stopped using opioids—whether because of jail time or treatment—are at increased risk of overdose, and we’ve heard inspiring stories of overdose reversals in these cases. While opioid addiction is a treatable disease, it is a chronic disease where relapse is unfortunately part of the natural history. Preventing overdose allows people to continue their progress towards recovery, and may enable them to seek out other lifesaving services.
What barriers stand in the way of implementing programs like this in other parts of the United States?
I’ll start first by listing features of the program in Massachusetts that contributed to its success and would support broader implementation: one is the use of a nasal delivery device for naloxone, allowing naloxone to be administered through the nose, instead of by injection. The other is a standing order issued by the health department that permits non-medical personnel to deliver overdose education and distribute naloxone. Without this order, a doctor would need to be present each time naloxone is given out. To date, there are still large parts of the country with no access to a lifesaving naloxone distribution program; though this program locator tool can help you find out if there is one near you.
The two main barriers to the expansion of these initiatives are that insurance companies do not cover the nasal delivery device that allows naloxone to be administered through the nose, and prescribers (doctors, nurse practitioners and physicians’ assistants) are not yet adequately educated on prescribing naloxone. We’ve created a website, prescribetoprevent.org, to help facilitate naloxone prescribing.
What message would you send to officials in countries like Russia and China where the death toll from drug overdoses continues to climb?
Preventing needless deaths from opioid overdose is a bridge issue – it’s a cause that people from different perspectives on treatment and harm reduction can agree and work together on. It can be a starting point from which we can work together in addressing the harms associated with drug use.
What happens now?
We keep implementing and evaluating this program and ones like it. In Massachusetts, overdose education and naloxone have been delivered to heroin users, prescription opioid users, patients in emergency departments, and the people who are most likely to respond to an overdose including: people who are incarcerated, family members, social service providers, police officers, and firefighters. It is important to determine how these programs should be tailored to different populations to maximize their reach, effectiveness and sustainability. That’s what we’re working on now.
Inspired by models like the one advanced by Dr. Walley, the Open Society Foundations supports efforts to distribute naloxone through harm reduction NGOs in a number of regions around the world, including China, Kyrgyzstan and the United States.
Roxanne Saucier is a researcher and analyst for the Open Society Public Health Program.