Avoiding Fatal Opiate Overdose
By Azzi Momenghalibaf
Shortly after Amy Winehouse was found dead in her London home in July, the media began speculating that a drug overdose was the likely culprit. The singer-songwriter’s struggles with drug use, particularly heroin, were well known and the media lost no time in making up its mind (incidentally, just this week, the results of a toxicology report showed that there were no illegal drugs in Winehouse’s system at the time of her death). But while the media was reporting on the dangers of drug overdose, a second, equally important story failed to make headlines: death from opiate overdose is easily avoidable with access to the lifesaving medicine, naloxone.
August 31st is International Overdose Awareness Day and an opportunity to raise awareness about drug use and harm reduction alternatives. Worldwide, between 12 and 21 million people use opiates for a variety of reasons. Many are prescribed opiates for pain or addiction. Others take them illicitly to deal with pain, because they have a habit, or because they want to get high. All are at risk of experiencing overdose—a leading cause of death among regular opiate users.
In the United States, opiate overdose is the second leading cause of accidental death, and in the European Union, the equivalent of one fatal overdose occurs every hour. Although data in many other countries is incomplete, surveys among drug users in places like Russia and Vietnam reveal that nearly all drug users have at one time witnessed a fatal overdose, and over a third have overdosed themselves. These numbers suggest that many of us know someone who has experienced an overdose—whether they’ve told us about it or not—including friends or family members. What most people don’t know—and what's rarely reported when a high-profile drug overdose (or in this case, a "suspected" drug overdose) makes the news—is information on naloxone.
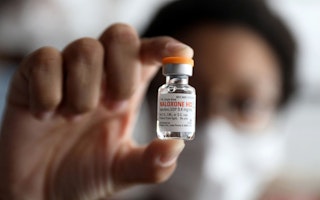
Naloxone is a safe, easy-to-use antidote to overdose from heroin or other opioids, like morphine, codeine, hydromorphone (vicodin), and oxycodone. Although naloxone has been used in emergency settings for decades, it is rarely available at that critical moment when people need it most. To maximize its lifesaving potential, harm reduction advocates, such as the Open Society Foundations, support "community or peer provision"—placing naloxone in the hands of those who are most likely to witness an overdose and respond first: opiate users, their families, and friends. Training more people in this basic first aid response, can help avoid death: it is as simple as that.
While we have seen that naloxone can be administered by just about anyone with minimal training, in many countries, legal and policy barriers prevent laypeople from administering it. Though naloxone is a remarkably safe medicine, many countries make it available only by prescription; others only allow certain medical professionals to inject it.
Opiate overdose is a looming crisis in our society that we can no longer ignore, and our responses to this problem should focus on reducing the risks associated with opiate use, in an effort to protect the health and human rights of all people who use opiates, in line with a harm reduction approach. Naloxone is at the heart of such an approach, particularly naloxone provision directly to drug users, pain patients, and their loved ones. Such programs are saving lives all over the world in countries like the United States, Russia, China, Tajikistan, Thailand, and Vietnam and should be expanded. Take for example that the Chicago Recovery Alliance has reversed over 2,000 overdoses with naloxone since they started community or peer distribution in 1996. In addition to the lifesaving potential of these programs, they have a profoundly empowering effect. Saving a life with naloxone provides a second chance and sends a clear message to drug users that their lives are worth saving.
Visit the Open Society Blog on August 31st to read testimonials from the frontlines on nalxone’s empowering effect, and learn what you can do to promote access to this lifesaving medicine.
Until November 2021, Azzi Momenghalibaf was a senior program officer with the Open Society Public Health Program.